The Difference Between Greening Out and THC Panic Attack: What You Need to Know

Nearly 1 in 5 cannabis users will experience a distressing reaction at some point, yet most people have no idea whether what they’re going through is a physical crisis, a mental health episode, or both. comprehending the difference between greening out and a THC panic attack could be the most important thing you read today, especially as cannabis products grow stronger and more widely available across New York.
These two experiences are often confused, and that confusion matters. One is primarily a physical overdose response. The other is primarily a psychological anxiety reaction. Both are real, both are scary, and both can be warning signs of a deeper relationship with cannabis that deserves attention.
Learn more with Expert Support for Substance Use in Brooklyn, NY.
Key Takeaways 🌿
- Greening out = a physical cannabis toxicity response (nausea, vomiting, dizziness, pallor)
- THC panic attack = a psychological anxiety response (racing heart, fear, derealization)
- Both can happen at the same time, making them easy to confuse
- Neither is a sign of weakness — both can signal problematic cannabis use
- Professional support is available, effective, and nothing to be ashamed of
Comprehending the Difference Between Greening Out and THC Panic Attack
What Is “Greening Out”?
“Greening out” is informal slang for what clinicians classify as acute cannabis intoxication or an adverse reaction to cannabis. It happens when someone consumes more THC than their body can comfortably process, essentially a cannabis overdose, though not typically life-threatening.
Common physical symptoms include:
- 🤢 Nausea and vomiting
- 😰 Profuse sweating and clamminess
- 😶 Pale or greenish skin tone
- 💫 Dizziness and loss of balance
- 🫀 Rapid or irregular heartbeat
- 🥴 Feeling faint or losing consciousness briefly
The person may feel physically terrible but may not be overwhelmed by fear. They often just want to lie down, stop moving, and wait it out. The body is reacting to a chemical overload, not necessarily a psychological spiral.
Greening out is more common with:
- Edibles (delayed onset leads to accidental overconsumption)
- High-potency concentrates or dabs
- First-time or low-tolerance users
- Mixing cannabis with alcohol
What Is a THC Panic Attack?
A THC panic attack is clinically described as a cannabis-induced anxiety disorder — a panic attack triggered or intensified by THC. Unlike greening out, the dominant experience here is overwhelming psychological fear, not primarily physical illness.
Common symptoms include:
- 😱 Intense, sudden terror or sense of doom
- ❤️ Racing or pounding heartbeat (palpitations)
- 😮💨 Shortness of breath or feeling smothered
- 🧠 Derealization (“this isn’t real”) or depersonalization
- 😨 Fear of dying or “going crazy”
- 🤲 Trembling, tingling, or numbness
THC is known to amplify the brain’s threat-detection systems. In people with underlying anxiety, a genetic predisposition, or past trauma, even a moderate dose can flip a switch from relaxed to terrified within minutes.
Side-by-Side Comparison: Greening Out vs. THC Panic Attack
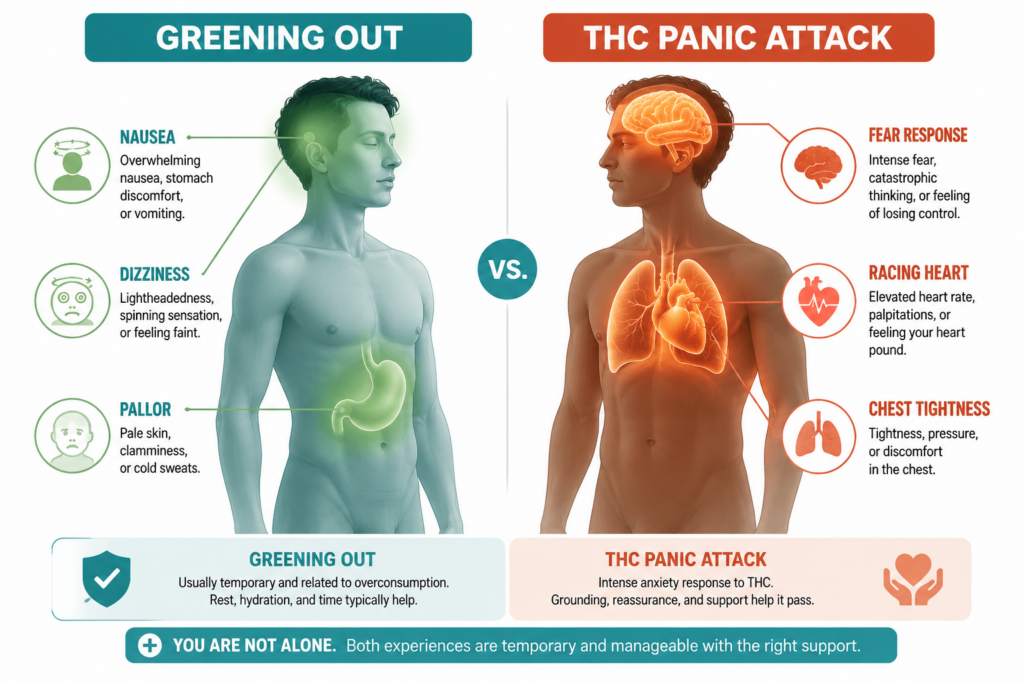
| Feature | Greening Out | THC Panic Attack |
|---|---|---|
| Primary nature | Physical / physiological | Psychological / emotional |
| Main complaint | Nausea, dizziness, vomiting | Fear, doom, derealization |
| Heart racing? | Sometimes | Very common |
| Vomiting? | Very common | Rare |
| Pale/sweaty skin? | Yes | Less typical |
| Sense of terror? | Mild or absent | Severe |
| Clinical term | Cannabis intoxication | Cannabis-induced anxiety disorder |
| Can they overlap? | ✅ Yes, frequently | ✅ Yes, frequently |
Can Both Happen at Once?
Yes, and this is where things get complicated. Many people experience both simultaneously. The physical misery of greening out can trigger panic, and the psychological spiral of a panic attack can worsen physical symptoms like nausea and heart rate. When they overlap, it can feel like a complete breakdown of mind and body.
This overlap is one reason why knowing how substance abuse can lead to mental illness is so important. Cannabis use can genuinely alter anxiety thresholds over time.
Why This Distinction Matters for Your Health
The Risk of Dismissing Either Experience
Both greening out and THC panic attacks are often brushed off as “just weed” — a dangerous minimization. Here’s why both deserve serious attention:
Greening out signals:
- Your body’s tolerance and physical limits are being exceeded
- You may be using higher-potency products than your system can handle
- Repeated episodes can indicate escalating use patterns
THC panic attacks signal:
- Your brain’s anxiety response may be dysregulated
- You may have an underlying anxiety disorder being masked or worsened by cannabis
- Cannabis may be functioning as a coping mechanism for unaddressed stress or trauma
If you’re regularly experiencing either, it’s worth exploring the stages of substance use to understand where your relationship with cannabis currently stands.
When Cannabis Use Becomes a Co-Occurring Issue 🔍
For many people, cannabis use doesn’t exist in a vacuum. It often co-occurs with anxiety disorders, depression, PTSD, or other mental health conditions. This is sometimes called a dual diagnosis or MICA (Mentally Ill Chemical Abuser) presentation.
Comprehending what MICA means in mental health can help people recognize that their cannabis-related distress may be part of a larger picture that deserves integrated, compassionate care.
What to Do During a Greening Out or THC Panic Attack
Immediate Steps for Greening Out
- Stop consuming — no more cannabis, no alcohol
- Lie down in a safe, quiet space
- Hydrate slowly — small sips of water or juice
- Eat something light if possible (sugar can help)
- Stay with someone you trust
- Call 911 if the person loses consciousness or can’t be roused
Immediate Steps for a THC Panic Attack
- Ground yourself — name 5 things you can see, 4 you can touch
- Breathe slowly — inhale for 4 counts, exhale for 6
- Remind yourself — “This is THC. It will pass. I am not dying.”
- Move to a calm environment — reduce stimulation
- Talk to someone — a calm, trusted voice helps enormously
- Seek emergency care if symptoms don’t subside or feel medically serious
The Difference Between Greening Out and THC Panic Attack: Long-Term Patterns to Watch
When Occasional Episodes Become a Pattern
A single bad experience with cannabis doesn’t define your relationship with it. But when these episodes happen repeatedly, or when you find yourself using cannabis to manage anxiety that cannabis itself is worsening, that cycle is worth examining honestly.
Signs that a pattern may be developing:
- Using cannabis daily to feel “normal” or calm
- Needing more to get the same effect (tolerance)
- Greening out more than once
- Panic attacks that happen even when sober
- Using cannabis to cope with trauma, stress, or emotional pain
Cannabis Detox: What to Expect
If you’ve decided to take a break or stop altogether, it helps to know what the process looks like. Knowing how long it takes to detox from cannabis can reduce anxiety about the withdrawal process and help you plan with realistic expectations.
Getting Support in Brooklyn: You Don’t Have to Figure This Out Alone

If any of this resonates — whether you’ve had a frightening greening out episode, recurring THC panic attacks, or you’re just questioning your relationship with cannabis — support is closer than you think.
At LSA Recovery Inc., we offer compassionate, stigma-free outpatient treatment for cannabis use and co-occurring mental health conditions across three Brooklyn locations:
- 📍 Midwood (Kings Highway): 1623 Kings Hwy, Brooklyn, NY 11229 — ☎️ (718) 954-3800
- 📍 Crown Heights: 921 E New York Ave, Brooklyn, NY 11203 — ☎️ (718) 684-7774
- 📍 Coney Island: 2846 Stillwell Ave, Brooklyn, NY 11224 — ☎️ (718) 975-2252
Our MICA program is specifically designed for people navigating both substance use and mental health challenges — because those two things almost always travel together. We also offer individual, family, and group counseling, substance use education, and care management to support every dimension of your recovery.
Same-day appointments are available. Telehealth options are available. Medicaid, Medicare, and most insurances accepted, and our insurance representatives can help if you’re still in the process of getting coverage.
FAQs:
Can greening out cause lasting physical harm?
In most cases, greening out resolves on its own within a few hours without permanent physical damage. Nonetheless severe vomiting can lead to dehydration, and in rare cases, very high THC doses have been associated with cannabinoid hyperemesis syndrome (CHS) a condition involving cyclical, severe vomiting. If symptoms are extreme or don’t resolve, seek emergency medical care.
Does having a THC panic attack mean I have an anxiety disorder?
Not necessarily, but it’s worth exploring. THC can trigger panic responses even in people without a clinical anxiety disorder, especially with high-potency products. Nevertheless, if panic attacks happen frequently, occur outside of cannabis use, or significantly disrupt your daily life, a proper mental health evaluation is strongly recommended.
Is cannabis use disorder a real diagnosis?
Yes. Cannabis use disorder (CUD) is a recognized clinical diagnosis in the DSM-5. It involves continued cannabis use despite negative consequences, tolerance, withdrawal symptoms, and difficulty cutting back. It exists on a spectrum from mild to severe. Recognizing it is not about shame — it’s about accessing the right level of support.
How do I know if I need professional help for cannabis-related anxiety?
Consider reaching out if: your cannabis use feels out of control, you’re using it primarily to manage anxiety or emotional pain, you’ve had multiple greening out or panic episodes, or your mental health has worsened alongside your use. You don’t need to hit a “rock bottom” to deserve support.
References
- Substance Abuse and Mental Health Services Administration (SAMHSA). (2023). Key substance use and mental health indicators in the United States: Results from the 2022 National Survey on Drug Use and Health. U.S. Department of Health and Human Services. https://www.samhsa.gov/data/report/2022-nsduh-annual-national-report
- National Institute on Drug Abuse (NIDA). (2024). Cannabis (marijuana) DrugFacts. National Institutes of Health. https://nida.nih.gov/publications/drugfacts/cannabis-marijuana
- Centers for Disease Control and Prevention (CDC). (2023). Health effects of marijuana. U.S. Department of Health and Human Services. https://www.cdc.gov/marijuana/health-effects/index.html
- American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed., text revision). https://www.psychiatry.org/psychiatrists/practice/dsm
- National Alliance on Mental Illness (NAMI). (2023). Marijuana and mental health. https://www.nami.org/About-Mental-Illness/Common-with-Mental-Illness/Substance-Use-Disorders
Expert Support for Substance Use in Brooklyn, NY: Your Complete Guide to LSA Recovery

Nearly 1 in 7 Americans will develop a substance use disorder at some point in their lives — yet fewer than 1 in 10 ever receive treatment. In Brooklyn, a borough of more than 2.5 million people, that gap between need and care is felt every single day. If you or someone you love is struggling, finding expert support for substance use is not a sign of weakness. It is one of the most courageous decisions a person can make.
At LSA Recovery Inc., Brooklyn residents have access to a medically supervised, compassionate outpatient program built around one belief: every person deserves a path to recovery that is free of shame, judgment, and blame. This guide walks you through what that support looks like, who it serves, and how to take the first step.
Start with Expert Support for Substance Use in Brooklyn, NY.
Key Takeaways 🗝️
- Expert support for substance use is available in Brooklyn through LSA Recovery’s three outpatient locations in Midwood, Crown Heights, and Coney Island.
- Services range from individual counseling and Medication-Assisted Treatment (MAT) to family therapy, crisis management, and vocational support.
- Same-day appointments, telehealth options, and multilingual staff make care accessible to nearly everyone.
- Medicaid, Medicare, and most insurances are accepted — with on-staff insurance representatives to help.
- Recovery is a personal journey; LSA Recovery supports all paths, including harm reduction.

Why Expert Support for Substance Use Matters in Brooklyn
Substance use disorders do not discriminate. They affect people of every age, background, income level, and zip code. In Brooklyn’s dense, diverse communities, the pressures of poverty, trauma, housing instability, and systemic inequality can all increase vulnerability to chemical dependency.
“Addiction is often rooted in trauma — not a lack of willpower.”
Comprehending this is the foundation of effective care. When someone receives expert support for substance use from trained professionals who see the whole person, not just the substance, recovery becomes not just possible, but sustainable.
Here is a quick look at why professional outpatient treatment makes a real difference:
| Without Treatment | With Expert Support |
|---|---|
| Cycles of relapse without tools to break them | Evidence-based strategies to manage triggers |
| Isolation and shame | Community, counseling, and connection |
| Untreated co-occurring mental health issues | Integrated dual-diagnosis care |
| Limited access to medical support | Medication-Assisted Treatment (MAT) available |
| Navigating systems alone | Care managers to coordinate all support |
If you want to understand more about what the recovery process looks like from the beginning, our guide to understanding the 5 stages of substance abuse is a helpful starting point.
Who Does LSA Recovery Serve?
LSA Recovery’s doors are open to a wide range of individuals, including:
- ✅ Adults struggling with alcohol, opioids, or other substance use disorders
- ✅ Individuals with co-occurring mental health conditions (MICA)
- ✅ Family members and loved ones of people in active addiction
- ✅ People involved in the criminal justice system
- ✅ Parents and caretakers referred through NYC’s Administration of Children’s Services (ACS)
- ✅ Anyone referred through DWI/DUI programs
- ✅ People of all insurance statuses — including those still obtaining coverage
Programs are conducted in English, Spanish, Russian, and Ukrainian, reflecting the rich diversity of Brooklyn’s communities.
A Full Spectrum of Expert Support for Substance Use
One of LSA Recovery’s greatest strengths is the breadth of its services. Rather than a one-size-fits-all approach, every client receives a customized treatment plan built around their specific needs, history, and goals.
🔍 Comprehensive Assessment
Every journey begins with an honest, non-judgmental evaluation. LSA’s experienced counselors conduct thorough substance use assessments to determine the right level of care and the most effective treatment path. You can also read our essential guide to substance abuse evaluations for recovery to know what to expect before your first appointment.
🧠 Individual, Family & Group Counseling
Healing rarely happens in isolation. LSA offers evidence-based counseling in three formats:
- Individual counseling — One-on-one sessions to explore personal history, triggers, and goals
- Family therapy — Rebuilding relationships and communication with loved ones
- Group therapy — Peer support that reduces isolation and builds community
Research consistently shows that group therapy supports long-term recovery by creating accountability and shared comprehension. Family sessions are equally powerful, learn more about LSA’s family therapy services in Brooklyn.
💊 Medication-Assisted Treatment (MAT) for Opioid Addiction
For individuals recovering from opioid addiction, Medication-Assisted Treatment is one of the most evidence-based tools available. MAT combines FDA-approved medications with counseling to reduce cravings, prevent withdrawal, and support sustained recovery. It is not a crutch, it is proven medicine.
🤝 Care Management
Recovery involves more than just treatment sessions. LSA’s care managers assess the full range of a patient’s needs — from housing and healthcare coordination to social services, and serve as a consistent point of contact throughout the recovery process. For more on how to access this kind of support, see our guide on how to access a mental health case manager.
🧩 MICA Program: Dual Diagnosis Support
Many people struggling with substance use also live with mental health conditions like depression, anxiety, PTSD, or bipolar disorder. LSA’s MICA Program (Mentally Ill Chemical Abuser) is specifically designed for individuals facing both challenges at once. Comprehending how substance abuse can lead to mental illness is critical to effective treatment.
LSA Recovery is also affiliated with Interborough Developmental & Consultation Center, a full mental health provider, allowing for seamless referrals when additional behavioral health support is needed.
🚨 Crisis Management
When someone is in acute crisis, they need immediate, compassionate support. LSA’s crisis management services provide short-term stabilization tools to help clients navigate emergencies safely without judgment.
📚 Additional Services at a Glance
| Service | Who It Helps |
|---|---|
| Substance Use Education | Clients learning to understand triggers and build drug-free living skills |
| Criminal Justice Counseling | Individuals navigating the legal system alongside recovery |
| DWI Program | Those charged with DWI/DUI infractions |
| ACS Program | Parents/caretakers referred through NYC’s child welfare system |
| Naloxone Training & Kits | Anyone at risk of opioid overdose or caring for someone who is |
| ACRA & CRAFT Program | Families trying to support a loved one who refuses treatment |
| Education & Vocational Services | Clients rebuilding careers and financial independence |
| HIV/AIDS Education | Prevention, risk reduction, and support for those diagnosed |
| Health Education Groups | Knowing how addiction impacts overall health |
Three Convenient Locations Across Brooklyn
LSA Recovery operates three outpatient locations to serve Brooklyn’s communities where they live.
📍 Midwood (Kings Highway)
1623 Kings Hwy, Brooklyn, NY 11229
📞 (718) 954-3800
Located within 2 blocks of the Q and B trains to Kings Highway, and accessible via the B7, B82, B68 & B100 bus lines.
Hours: Mon, Wed, Thu: 8:30 AM–8:00 PM | Tue: 8:30 AM–5:00 PM | Sun: 9:00 AM–5:00 PM
📍 Crown Heights
921 E New York Ave, Brooklyn, NY 11203
📞 (718) 684-7774
Hours: Mon: 9:00 AM–8:00 PM | Tue–Thu: 9:00 AM–5:00 PM
📍 Coney Island
2846 Stillwell Ave, Brooklyn, NY 11224
📞 (718) 975-2252
Hours: Tue & Thu: 9:00 AM–8:00 PM | Mon, Wed: 9:00 AM–5:00 PM
Telehealth appointments are available Monday–Thursday from 7:00 AM–11:00 PM and Sunday from 9:00 AM–7:00 PM — making expert support accessible even when getting to an office is difficult.
Insurance & Access: No Barrier Should Stand in the Way
One of the most common reasons people delay seeking help is fear about cost. LSA Recovery accepts Medicaid, Medicare, and most private insurance plans. For those who are still in the process of obtaining coverage, insurance representatives are on staff to help navigate the system.
Same-day appointments are available. There is no reason to wait.
📧 Email: info@lsarecovery.org
🌐 Book online: lsarecovery.org/contact-us
Your Recovery Starts With One Step
In 2026, the conversation around substance use is changing. More people are recognizing that addiction is a medical condition — one that responds to compassionate, evidence-based care. Brooklyn has the resources, and LSA Recovery Inc. is here to provide the expert support for substance use that you or your loved one deserves.
Here are your actionable next steps:
- 📞 Call the LSA Recovery location nearest to you — same-day appointments are available.
- 🌐 Visit lsarecovery.org/contact-us to book an appointment online.
- 📋 Start with a comprehensive assessment — no commitment, no judgment, just honest guidance.
- 💬 Bring a family member — recovery is stronger when loved ones are involved.
- 🛡️ Ask about insurance — an on-staff representative can help you figure out your coverage today.
Recovery is not a straight line, and there is no single right path. What matters is that you take the first step, and that you do not take it alone.
Is Naltrexone the Same as Naloxone? A Clear Guide for Patients and Family Members
They sound identical, but confusing these two medications could be a matter of life or death. When navigating addiction, families constantly ask: Is naltrexone the same as naloxone? One acts as a daily shield for long-term sobriety, while the other is a rapid emergency lifesaver. Uncover the crucial differences in this guide to ensure you know exactly which one to use before it matters most.
Access knowledge via Naloxone Training
TL;DR:
Naltrexone is a non-addictive medication used to treat opioid and alcohol use disorders by actively blocking the brain’s opioid receptors, which suppresses cravings and neutralizes the euphoric effects of substance use. Available in either a daily oral form or a monthly extended-release injection, the medication is most effective when utilized as part of a comprehensive recovery plan that includes behavioral counseling and peer support. To avoid triggering sudden and severe withdrawal symptoms, patients must be completely opioid-free for 7 to 14 days before initiating treatment.

What is Naltrexone and How does it Work?
Naltrexone is a medication commonly utilized in the treatment of opioid use disorder (OUD) and alcohol use disorder (AUD). It belongs to a class of medications known as opioid antagonists, which means it works by actively blocking opioid receptors in the brain. Unlike opioid medications, naltrexone does not produce euphoric or sedative effects, nor is it considered addictive. It is typically utilized as one component of a broader, comprehensive recovery plan that includes counseling, behavioral therapy, and ongoing medical support.
The medication functions by attaching to opioid receptors without actually activating them. This prevents opioids from producing the pleasurable effects that drive misuse and dependence. National mental health and substance abuse authorities note that naltrexone can effectively reduce cravings and support long-term recovery outcomes. Furthermore, clinical research indicates that when combined with comprehensive care, medications for opioid use disorder improve treatment retention and reduce the risk of overdose.
Naltrexone is also widely used for alcohol dependence. Studies suggest that by blocking opioid pathways, the medication reduces the rewarding sensations associated with alcohol consumption, which helps individuals decrease heavy drinking episodes and maintain sobriety. Because introducing naltrexone while opioids are still in the body can trigger sudden and severe withdrawal symptoms, medical professionals strongly recommend using it under careful supervision, ensuring the patient is completely opioid-free before beginning treatment.
Blocking Opioid Receptors to Prevent Effects
One of naltrexone’s primary functions is its ability to block the brain’s mu-opioid receptors, which are responsible for producing feelings of pain relief and euphoria. If an individual takes opioids while naltrexone is active in their system, the medication prevents those substances from binding effectively to the receptors. As a result, the user does not experience the pleasurable “high” that reinforces continued opioid misuse.
This blocking action is a vital component of relapse prevention. Because the medication interrupts the cycle of reinforcement by neutralizing the euphoric and sedative effects of opioids, individuals recovering from addiction may be less likely to continue using them.
It is important to note that naltrexone differs from medications like methadone or buprenorphine because it blocks opioid activity rather than replacing opioids. Naltrexone does not cause physical dependence, and stopping it does not typically result in withdrawal symptoms.
Reducing Cravings and Risk of Relapse
Cravings represent one of the most significant challenges in addiction recovery, as the brain continues to associate substances with pleasure and emotional relief. Naltrexone is frequently used to suppress these cravings and lower the risk of relapse. By blocking opioid receptors, it reduces the rewarding sensations tied to substance use, helping to decrease the urge to use again.
Public health and substance abuse authorities view naltrexone as a valuable tool for individuals who have completed detoxification and are committed to maintaining their recovery. Healthcare providers frequently incorporate it into long-term relapse prevention plans because combining medication-assisted treatment with behavioral support tends to decrease relapse rates.
- Overdose Vulnerability: Relapse prevention is particularly critical because patients who discontinue naltrexone and return to opioid use are highly vulnerable to overdose. This heightened risk occurs because the body’s opioid tolerance significantly drops during a period of abstinence.
- Improving Engagement: To improve treatment engagement, recent federally supported clinical trials have explored faster initiation protocols for extended-release injectable naltrexone, demonstrating ongoing efforts to make recovery treatments more accessible and effective.
Supporting Long-Term Recovery Treatment
Addiction is a chronic medical condition that often involves periods of relapse and recovery, meaning long-term success requires more than just short-term detoxification. Naltrexone is commonly integrated into a “whole-patient approach” designed to address both the psychological and physical aspects of addiction. This helps individuals maintain abstinence while they actively develop healthier coping strategies and lifestyle changes.
Healthcare professionals frequently pair naltrexone with mental health services, peer support, and family counseling. This integrated model helps individuals rebuild their routines, relationships, and emotional stability. Research shows that medication-based approaches for opioid use disorder can reduce overdose deaths, improve treatment retention, decrease behaviors linked to infectious disease transmission, and support overall quality of life, including employment and family functioning.
Administering Oral or Injectable Forms
Naltrexone is available in two formulations, allowing providers to tailor the treatment to a patient’s specific recovery goals. The choice between oral and injectable forms is based on the patient’s medical history, access to treatment, and personal preference. Recent clinical studies also suggest that accelerating the initiation of the injectable form (beginning within five to seven days of seeking care) may improve treatment success compared to longer waiting periods, though it requires enhanced medical oversight.
| Formulation Type | Administration & Frequency | Considerations & Best Use |
| Oral Form | Typically taken once daily. | Common for alcohol dependence treatment. Appropriate for individuals who can consistently maintain a daily schedule. Missing doses increases the risk of relapse. |
| Extended-Release Injectable | Administered by a professional approximately once every four weeks. | Approved for both opioid and alcohol use disorders. Removes the need for daily dosing decisions, improving overall treatment consistency. |
Monitoring Use Under Medical Supervision
Given the risks associated with early initiation, medical supervision is a critical component of naltrexone treatment. Before starting, patients undergo an evaluation—which may include urine drug screenings or a naloxone challenge test—to confirm that their body is completely free of opioids.
General health guidelines advise waiting at least seven days after using short-acting opioids, and up to 10 to 14 days after using long-acting opioids, before taking naltrexone. Starting too soon can trigger severe withdrawal symptoms requiring immediate medical intervention.
Ongoing monitoring allows healthcare teams to manage side effects, track recovery progress, and monitor liver function and mental health. A vital part of this supervision involves educating patients about their lost opioid tolerance and the severe overdose risk if they relapse after stopping the medication. By addressing the individual’s overall physical, social, and emotional needs through continuous monitoring and coordinated counseling, healthcare providers can greatly reduce the likelihood of future relapse and support lasting recovery.
Key Takeaways:
- Mechanism of Action and Cravings: Naltrexone is a non-addictive medication used to treat opioid and alcohol use disorders by actively blocking the brain’s mu-opioid receptors. By neutralizing the euphoric and sedative effects of these substances, it effectively suppresses intense cravings and interrupts the cycle of reinforcement to prevent relapse.
- The Necessity of Prior Detoxification: Patients must be completely opioid-free for 7 to 14 days before beginning naltrexone, as starting the medication too early can trigger sudden, severe withdrawal symptoms. Because of this inherent biological risk, initiating the treatment requires strict medical supervision and pre-evaluations like urine screenings.
- Integrated Long-Term Recovery: Addiction is a chronic condition that requires a “whole-patient approach,” meaning naltrexone is most effective when combined with comprehensive behavioral support. Pairing the medication with mental health services, peer support, and family counseling helps individuals maintain abstinence while rebuilding their routines and emotional stability.
- Adaptable Administration Options: Treatment can be tailored to a patient’s needs through either a daily oral pill or a monthly extended-release injection. While the daily oral form requires strict adherence to remain effective, the injectable option removes daily dosing decisions and significantly improves overall treatment consistency.
- Overdose Vulnerability and Monitoring: Continuous medical supervision is crucial to manage side effects, track progress, and educate patients on their significantly lowered opioid tolerance during recovery. This education is a matter of life or death, as relapsing after a period of naltrexone-assisted abstinence carries a severely heightened risk of fatal overdose.
FAQs:
What is naltrexone?
Naltrexone is a non-addictive medication commonly utilized to treat opioid use disorder (OUD) and alcohol use disorder (AUD). As an opioid antagonist, it works by actively attaching to and blocking opioid receptors in the brain, effectively preventing substances from producing the pleasurable, euphoric, or sedative effects that drive misuse.
What is the difference between naloxone and naltrexone?
While their names sound identical, confusing the two can be a matter of life or death because they serve entirely different roles in addiction management. The text distinguishes them by noting that one medication acts as a daily shield to help maintain long-term sobriety, while the other is utilized as a rapid emergency lifesaver.
What is naloxone?
Naloxone is a medication utilized as a rapid emergency lifesaver. Additionally, healthcare providers use it in a “naloxone challenge test” during a patient’s initial evaluation to confirm that their body is completely free of opioids before they begin other treatments.
What are naloxone and naltrexone used for?
Naltrexone is used to treat opioid use disorder (OUD) and alcohol use disorder (AUD) by acting as a daily shield to support long-term sobriety. It works by actively blocking opioid receptors in the brain to reduce cravings and prevent the pleasurable effects that drive misuse. In contrast, naloxone is used as a rapid emergency lifesaver and is also administered in clinical challenge tests to ensure a patient is entirely opioid-free before starting naltrexone therapy.
Sources.
National Institutes of Health. (2024, March 22). Faster approach for starting extended-release naltrexone to treat opioid use disorder shown effective. U.S. Department of Health and Human Services. https://www.nih.gov/news-events/news-releases/faster-approach-starting-extended-release-naltrexone-treat-opioid-use-disorder-shown-effective
Centers for Disease Control and Prevention. (2024, May 15). Recovery is possible: Treatment for opioid addiction. U.S. Department of Health and Human Services. CDC Overdose Prevention Page
You May Also Like:
Can You Overdose on Narcan? Risks and Facts Explained
Living with Chronic HIV Anxiety: How to Regain Your Quality of Life
You’ve taken the tests and heard the medical reassurances, yet the fear continues to dictate your every waking moment. Why does the mind refuse to let go even when the body is safe? This relentless cycle is exhausting, but a way out exists. Explore Living with Chronic HIV Anxiety: How to Regain Your Quality of Life and discover how professional HIV/AIDS training can finally help you break the loop.
Get informed with HIV/AIDS training
TL;DR:
Chronic HIV-related anxiety is an exhausting cycle fueled by the profound fear of a positive diagnosis, societal stigma, and a lack of accurate medical education. Sufferers frequently misinterpret normal, anxiety-induced physical symptoms as signs of infection and resort to compulsive reassurance-seeking, such as repetitive testing, which ultimately reinforces their fear rather than resolving it. Breaking this debilitating loop requires addressing the underlying psychological distress directly and replacing outdated myths with clear, evidence-based information.

What Causes Chronic HIV-related Anxiety?
Dealing with persistent worries about your health can be incredibly exhausting. Chronic HIV-related anxiety develops when fear about HIV becomes overwhelming and difficult to control over time. This heavy burden can affect people living with HIV, those waiting for test results, or even individuals who constantly worry about exposure despite receiving repeated negative tests and medical reassurance.
Often, this anxiety goes far beyond medical concerns, intertwining with deep emotional distress, social stigma, uncertainty, and misinformation. Research highlights that this intense worry can severely interfere with daily life, relationships, sleep, and overall well-being. Without the right support and accurate information, this cycle of fear can unfortunately last for months or even years.
Fear of Diagnosis and Health Uncertainty
One of the primary drivers of this anxiety is the profound fear of receiving a positive diagnosis or simply living with uncertainty about your health status. Health uncertainty is emotionally draining; waiting periods, confusion about risk levels, and catastrophic thinking can trigger a surge in stress hormones and disrupt sleep.
- Catastrophic Thinking: Even before a test is taken, many people experience intense worry about what an HIV diagnosis could mean for their future, relationships, and quality of life.
- Information Gaps: This fear is frequently magnified when individuals are unfamiliar with modern HIV treatments or when they rely on outdated information.
- Symptom Searching: While modern treatments have drastically improved long-term outcomes, constant worry can create a cycle where the uncertainty itself becomes the main source of distress, particularly if someone spends excessive time searching for symptoms online.
Stigma and Social Judgment Concerns
The fear of social judgment is a heavy weight to carry. Many individuals fear being judged, rejected, or discriminated against due to the cultural beliefs and negative public attitudes historically associated with HIV. This fear can be profound even for those who have never been diagnosed.
| Impact Area | Clinical Consequence |
| Shame and Isolation | Public health organizations note that the stigma surrounding HIV can lead to deep feelings of shame and isolation. |
| Healthcare Avoidance | It can actively discourage people from seeking healthcare, getting tested, or openly discussing their sexual health. |
| Testing Anxiety | Recent qualitative studies highlight that this fear of judgment and concerns about confidentiality significantly drive testing anxiety. Sadly, when stigma goes unaddressed, the emotional fear of judgment can persist long after a negative test result or successful treatment. |
Misinterpretation of Physical Symptoms
It is incredibly common for health anxiety to make you hyper-focused on your body. Anxiety itself can produce a wide range of physical symptoms—such as fatigue, sweating, headaches, nausea, muscle tension, dizziness, and sleep disturbances. Unfortunately, people often misinterpret these normal stress responses or minor unrelated illnesses as signs of an HIV infection.
Mental health research shows that anxiety disorders heighten our attention to perceived physical danger. This creates a vicious, reinforcing cycle: anxiety causes physical symptoms, and those physical symptoms in turn spike your anxiety.
Internet searches often worsen the problem by offering broad symptom lists without medical context. It is important to remember that HIV cannot be diagnosed based on symptoms alone.
Repetitive Testing and Reassurance Seeking
When anxiety takes hold, it’s natural to look for a quick way to feel better. This often leads to compulsive reassurance-seeking behaviors, such as taking multiple HIV tests well beyond recommended timelines, constantly checking the body for illness, or repeatedly searching symptoms online.
- Short-Term Relief: A negative test result might offer a brief moment of relief, but the doubts inevitably creep back in. You might start questioning the test’s accuracy or the timing windows.
- Reinforcing Fear: While testing is a vital medical tool, psychological research indicates that excessive reassurance-seeking actually reinforces fear rather than resolving it.
- Daily Disruption: Over time, this repetitive cycle drains your emotional energy and interferes with daily functioning. Healthcare professionals usually recommend addressing the underlying anxiety itself rather than relying on endless testing for temporary comfort.
Ongoing Stress From Lack of Clear Information
A lack of clear, understandable information can cause anxiety to spiral. Outdated beliefs, conflicting online advice, and myths about how HIV is transmitted often lead people to drastically overestimate their actual risk. Confusion regarding testing windows, prevention strategies, and modern treatment outcomes creates a breeding ground for constant doubt.
Without reliable medical communication, people tend to fall back on internet forums or anecdotal stories that only fuel their panic. Public health experts emphasize that clear, evidence-based education is essential.
Comprehending how transmission actually works and how effective modern treatments are can help you distinguish between realistic health concerns and anxiety-driven thoughts, ultimately helping to break the cycle of chronic fear.
Key Takeaways:
- Fear of Diagnosis and Uncertainty: Chronic anxiety is heavily driven by the profound fear of a positive diagnosis and the emotional exhaustion of living with health uncertainty. This distress is frequently amplified by catastrophic thinking and excessive online symptom searching, creating a vicious cycle of worry.
- The Impact of Stigma and Judgment: The persistent fear of social rejection, discrimination, and cultural stigma significantly contributes to deep feelings of shame and emotional isolation. This heavy burden actively discourages individuals from seeking necessary healthcare, openly discussing sexual health, or taking tests.
- Misinterpreting Physical Symptoms: Health anxiety frequently causes normal physical stress responses, such as fatigue, sweating, or muscle tension, to be incorrectly interpreted as definitive signs of an HIV infection. Because anxiety heightens attention to perceived physical danger, it creates a self-reinforcing cycle where panic triggers physical symptoms, which in turn spike further anxiety.
- The Trap of Reassurance Seeking: To temporarily relieve their intense worry, individuals often resort to compulsive reassurance-seeking behaviors, such as taking multiple unnecessary HIV tests or constantly checking their bodies. Psychological research indicates that this continuous cycle actually reinforces long-term fear rather than resolving the underlying uncertainty.
- Ongoing Stress from Misinformation: A severe lack of clear, evidence-based medical information creates a breeding ground for constant doubt and causes individuals to drastically overestimate their actual risk. Outdated beliefs, myths, and conflicting online advice fuel panic instead of offering clarity regarding transmission, testing windows, and modern treatments.
FAQs:
Can HIV trigger anxiety?
Yes, HIV and the profound fear surrounding it can absolutely trigger anxiety. Chronic HIV-related anxiety develops when fears about the condition become overwhelming, affecting individuals living with HIV, those waiting for test results, and even people who constantly worry about exposure despite receiving medical reassurance and negative tests.
How to get over HIV anxiety?
To overcome this anxiety, healthcare professionals advise addressing the root psychological distress directly rather than relying on compulsive behaviors like endless testing, which only offer temporary comfort and ultimately reinforce fear. A critical step in breaking this cycle involves replacing outdated myths with clear, evidence-based medical education.
Is HIV anxiety common?
Yes, research shows that anxiety is a very common experience among people affected by HIV concerns. It is incredibly common for this health anxiety to cause individuals to become hyper-focused on their bodies, leading them to constantly monitor for changes and misinterpret normal stress responses or minor illnesses as signs of an infection.
Can stress worsen HIV?
Anxiety produces a wide range of physical symptoms, such as fatigue, sweating, muscle tension, and sleep disturbances, that individuals mistakenly attribute to an HIV infection. Catastrophic thinking triggers stress hormones that disrupt sleep, creating a vicious, self-reinforcing cycle where physical symptoms and anxiety continually spike one another.
Sources.
Owusu, A.Y. Experiences of new diagnoses among HIV-positive persons: implications for public health. BMC Public Health 22, 538 (2022). https://doi.org/10.1186/s12889-022-12809-6
Iott, B.E., Loveluck, J., Benton, A. et al. The impact of stigma on HIV testing decisions for gay, bisexual, queer and other men who have sex with men: a qualitative study. BMC Public Health 22, 471 (2022). https://doi.org/10.1186/s12889-022-12761-5
Parsons, C. A., & Alden, L. E. (2022). Online reassurance-seeking and relationships with obsessive-compulsive symptoms, shame, and fear of self. Journal of Obsessive-Compulsive and Related Disorders, 33, 100714.
You May Also Like:
Differences Between Detox and Rehabilitation in Recovery
You might think quitting is just a test of willpower, but what if your own body is actively working against you? The hidden biological reality of withdrawal holds dangers that most people completely ignore. Uncover the truth in What is Detox and How does It Work? and discover why a professional Chemical Dependency Assessment is the ultimate missing link for a safe, lasting recovery.
Start with a Chemical Dependency Assessment.
TL;DR:
Detoxification is the vital, medically supervised first step in addiction recovery, designed to safely clear harmful substances from the body while managing severe and potentially dangerous physical withdrawal symptoms. Through continuous monitoring, evidence-based medications, and compassionate emotional support, professional detox programs stabilize patients both physically and psychologically. Nevertheless, detox is not a standalone cure; rather, it serves as a critical, short-term launching pad that prepares individuals to successfully transition into the long-term rehabilitation and therapy programs necessary for lasting sobriety.

What is Detox and How does It Work?
Detoxification, or detox, is the crucial first stage of treatment for substance use disorders. It is the process in which the body clears itself of alcohol, drugs, or other harmful substances while medical professionals manage the physical and emotional effects of withdrawal. General health guidelines emphasize that detox is not a “cure” for addiction on its own; rather, it is a stabilizing first step designed to prepare individuals for longer-term therapy and recovery support.
When a person suddenly stops using substances after prolonged exposure, the brain and body must adjust. This sudden absence can trigger withdrawal symptoms ranging from anxiety and nausea to severe complications like seizures or cardiovascular instability. Because of these inherent risks, professional detox programs, which can take place in hospitals, residential centers, or outpatient settings, are highly recommended to ensure patient safety.
Removing Substances From the Body Safely
While the body naturally processes and eliminates toxins through organs like the liver and kidneys, the accompanying withdrawal phase can be physically and emotionally overwhelming. Professional programs provide a controlled environment to safely manage this elimination process.
The length of detox varies widely depending on the type of substance used, the duration and amount of use, and the individual’s overall health. For substances like alcohol and benzodiazepines, withdrawal can become life-threatening without medical supervision. To ensure safety and comfort, healthcare providers may administer evidence-based medications to reduce cravings, alongside providing vital hydration, nutritional support, and rest.
Managing Withdrawal Symptoms Medically
As substances leave the body, the brain and nervous system react abruptly to the sudden absence of chemicals they had become dependent on. This adjustment period often causes a variety of physical and psychological symptoms that require close supervision. The severity of these symptoms heavily depends on the specific substance involved and the person’s unique medical history, ranging from mild discomfort to severe medical emergencies.
- Common Symptoms: Nausea, headaches, sweating, anxiety, insomnia, irritability, muscle pain, tremors, and intense cravings.
- Severe Emergencies: Hallucinations, seizures, respiratory complications, and dangerously elevated blood pressure.
Medical management utilizes continuous monitoring and evidence-based interventions to ease this discomfort, stabilize the patient, and prevent severe complications. For example, healthcare providers may administer specific medications during opioid withdrawal to decrease cravings and improve treatment retention, while medications for alcohol withdrawal are used to reduce the risk of agitation and life-threatening seizures.
Furthermore, emotional and psychological support is a crucial component of this phase. Staff members provide counseling, reassurance, and crisis intervention to help patients navigate the fear, depression, or emotional distress that frequently accompany withdrawal. According to SAMHSA, combining these medications with counseling and behavioral therapies often creates significantly better treatment outcomes and actively supports long-term recovery.
Monitoring Vital Signs and Stabilization
Patient safety during detox relies heavily on the close, continuous observation of vital signs. Because withdrawal can severely affect multiple body systems, medical observation becomes exceptionally important in moderate to severe cases.
Medical teams actively monitor vital signs such as heart rate, blood pressure, body temperature, oxygen levels, and breathing patterns. They also evaluate the patient’s hydration, sleep patterns, mental status, and neurological symptoms. Any sudden changes in these critical indicators can quickly signal developing complications that require immediate medical intervention.
The major goal of this entire phase is stabilization, helping the patient reach a medically and emotionally stable condition before they move into ongoing treatment. This comprehensive stabilization process involves:
- Administering necessary medications.
- Treating dehydration and improving overall nutrition.
- Managing co-occurring conditions, such as anxiety disorders, depression, trauma, or chronic illnesses that need simultaneous attention.
Withdrawal symptoms and cravings can be incredibly intense, especially during the first few days. By maintaining a highly structured and supervised environment, treatment professionals can respond rapidly to patient needs, provide continuous encouragement, and greatly reduce the risk of relapse during this highly vulnerable stage of early recovery.
Providing Short-Term Clinical Support
Detox is a short-term clinical intervention designed specifically to help patients navigate the earliest, most difficult stage of recovery. The support provided here, including physician care, nursing supervision, and mental health services, can significantly influence a person’s readiness to continue treatment.
Many individuals enter detox experiencing feelings of shame, fear, or hopelessness. Compassionate clinical care helps alleviate this stigma, reinforcing that substance use disorder is a treatable condition rather than a moral failing. This short-term phase concludes with careful discharge planning to prepare the patient for what comes next.
Preparing for Ongoing Treatment Programs
Detoxification is most effective when it serves as the launching pad for a larger, long-term recovery plan. Because detox alone rarely addresses the underlying psychological or behavioral causes of addiction, patients are encouraged to transition directly into structured ongoing treatment.
Depending on the individual’s specific needs and goals, ongoing care may include:
- Inpatient rehabilitation or outpatient therapy
- Medication-assisted treatment
- Group, individual, or family counseling
- Peer support services
Before detox ends, healthcare providers collaborate with patients to build these personalized treatment plans. Through education on stress management, coping strategies, and relapse triggers, individuals are equipped with the necessary tools and support systems to sustain their long-term recovery journey.
Key Takeaways:
- The Foundational Role of Detox: Detoxification serves as the essential first stage in addiction treatment, focusing on safely clearing substances from the body while stabilizing the patient. It is not a standalone cure, but rather a vital clinical intervention designed to prepare individuals for comprehensive rehabilitation.
- Medical Management of Withdrawal: Abruptly stopping prolonged substance use triggers withdrawal symptoms that range from mild anxiety to life-threatening emergencies like seizures. To mitigate these risks, medical management relies on continuous monitoring and the administration of evidence-based medications to ease discomfort and reduce intense cravings.
- Vital Sign Monitoring and Stabilization: Patient safety heavily depends on the continuous observation of vital signs, including heart rate, blood pressure, and oxygen levels. The ultimate goal of this phase is complete stabilization, achieved by treating dehydration, improving nutrition, and managing any co-occurring mental health disorders.
- Short-Term Emotional and Clinical Support: The withdrawal phase is frequently accompanied by profound emotional distress, with patients entering detox experiencing deep fear, depression, or shame. Compassionate clinical care provides crucial counseling and crisis intervention to alleviate this stigma, treating addiction as a medical condition rather than a moral failing.
- Transitioning to Long-Term Treatment: Because detox alone rarely resolves the underlying behavioral causes of addiction, it must serve as a launching pad for structured, long-term recovery plans. Healthcare providers collaborate closely with patients before discharge to transition them into inpatient rehabilitation, outpatient therapy, or peer support services.
FAQs:
What is the difference between detoxification and rehabilitation?
Detoxification is the crucial first stage of recovery focused on safely clearing harmful substances from the body and medically managing the physical and emotional symptoms of withdrawal. Rehabilitation is the structured, longer-term phase of ongoing treatment that follows detox, specifically designed to address the underlying psychological and behavioral causes of addiction.
What is the meaning of detox in rehabilitation?
In the context of rehabilitation, detox serves as a stabilizing first step rather than a standalone cure. It is a short-term clinical intervention intended to help patients safely navigate the dangerous biological realities of withdrawal, acting as the essential launching pad to prepare them physically and emotionally for ongoing therapy.
What does rehabilitate mean?
To rehabilitate means to engage in a comprehensive, long-term recovery plan that treats the behavioral, emotional, and psychological aspects of addiction. It involves equipping patients with the necessary tools, such as stress management skills and coping strategies for relapse triggers, to sustain their sobriety and improve their overall health, wellness, and quality of life.
What is an example of rehabilitation?
Examples of rehabilitation include structured ongoing treatment programs such as inpatient rehabilitation or outpatient therapy. Depending on an individual’s specific needs, this care can also involve medication-assisted treatment, individual psychotherapy, group and family counseling, and peer support services.
Sources.
Centers for Disease Control and Prevention. (2024, May 15). Treatment of substance use disorders. U.S. Department of Health and Human Services. https://www.cdc.gov/overdose-prevention/treatment/index.html
Centers for Disease Control and Prevention. (2024, May 7). Clinical care and treatment for substance use disorders. U.S. Department of Health and Human Services. CDC Overdose Prevention – Clinical Care and Treatment for Substance Use Disorders
You May Also Like:
The Pros and Cons of Prisoner Rehabilitation in the U.S.
Differences Between Types of Drug Tests: Urine, Saliva, Blood, Hair
You have an upcoming drug test and feel confident you’re in the clear, but what if the method they choose changes everything? Not all tests look for the same evidence, and one simple mistake could jeopardize your results. Discover the Differences Between Types of Drug Tests: Urine, Saliva, Blood, Hair, and learn why choosing a proper detox in Brooklyn might be the safety net you never knew you needed.
Find details at Detox in Brooklyn
TL;DR:
Urine drug tests are a reliable, noninvasive method used to detect recent substance use by identifying drug metabolites rather than the drugs themselves. The procedure relies on a strict, two-step laboratory process. After secure sample collection and validity checks to prevent tampering, an initial rapid screening (immunoassay) flags potential substances. Any presumptive positive results then undergo highly precise, advanced confirmatory testing (such as GC-MS) to eliminate false positives.

How does a Urine Drug Test Work?
A urine drug test is a relatively noninvasive, cost-effective laboratory procedure used to detect the presence of drugs or their metabolites in a person’s urine. Widely utilized in workplaces, healthcare settings, rehabilitation programs, athletic organizations, and legal investigations, it is highly effective at identifying recent substance use.
Rather than detecting the drug itself, these tests typically look for metabolites, substances created when the body breaks down a drug. Federally regulated programs commonly screen for substances like amphetamines, cocaine metabolites, marijuana metabolites, opioids, and phencyclidine. The testing generally follows a reliable two-step process: a rapid initial screening, followed by an advanced confirmatory test for any presumptive positives. This layered process, when interpreted alongside a patient’s medical history to account for cross-reactivity, greatly improves the accuracy of the results.
Sample Collection and Handling
Proper collection and handling are crucial, as improper procedures can easily compromise the validity of the results. Individuals provide a sample in a sterile container under controlled conditions to prevent contamination, substitution, or tampering.
- Chain-of-Custody: The sample is labeled and tracked using a strict process, documenting everyone who handles it from collection to analysis to prevent legal or workplace disputes.
- Validity Testing: Laboratories check the sample’s temperature, pH, creatinine concentration, and specific gravity to ensure it hasn’t been diluted or adulterated.
- Storage and Transportation: Samples are promptly refrigerated and transported under strict quality assurance protocols, as exposure to extreme temperatures or poor sealing can alter the chemical stability of the specimen.
Detection of Drug Metabolites
Urine tests primarily focus on detecting metabolites, which are produced when the liver chemically processes a substance. Because metabolites stay in the system longer than the parent drug, they act as a more reliable indicator of recent use.
| Factor | Description |
| Common Breakdowns | Public health organizations note that cocaine metabolizes into benzoylecgonine, while heroin breaks down into morphine and 6-monoacetylmorphine. |
| Detection Window | This depends on factors like dosage, frequency of use, hydration, body composition, and overall health—ranging from a day or two to several weeks for chronic use. |
| Cutoff Levels | Laboratories use specific concentration thresholds to determine a positive or negative result, helping to prevent false positives from trace environmental exposures. |
Laboratory Screening Process
The initial screening typically relies on immunoassay tests. These biochemical tests detect specific molecular structures associated with drug classes and are highly favored because they can process large volumes of samples rapidly and efficiently.
This initial step is qualitative, meaning it simply indicates if a substance may be present above the designated cutoff. Nevertheless, immunoassays are considered presumptive. Clinical literature highlights that cross-reactivity with certain prescription medications, over-the-counter products, or underlying medical conditions can occasionally cause false-positive or false-negative results.
If a screening returns a negative result, testing usually concludes. If it returns a presumptive positive, the sample advances to the next stage under strict professional standards.
Confirmation Through Advanced Testing
To verify a positive screen and accurately identify the exact drug or metabolite, laboratories employ highly sophisticated confirmatory tests.
- Gold Standard Methods: The most common methods are gas chromatography-mass spectrometry (GC-MS) and liquid chromatography-tandem mass spectrometry (LC-MS/MS).
- High Precision: These technologies separate chemical compounds and identify them by their unique molecular characteristics, drastically reducing the chance of a false positive.
- Quantitative Analysis: Furthermore, confirmatory testing measures the exact concentration of the metabolite to differentiate between true exposure and unrelated cross-reactivity.
- Medical Review: In regulated programs, specially trained physicians known as Medical Review Officers evaluate these confirmed findings alongside the patient’s medical and prescription history to ensure an accurate, fair interpretation.
Interpretation of Test Results
Interpreting a urine drug test requires analyzing the broader clinical context rather than just reading a “positive” or “negative” label. A positive result means a substance was detected above the cutoff level, but it does not inherently prove impairment or addiction. Conversely, a negative result only means the substance was absent or below the reporting threshold, not that the individual has never used drugs.
Medical literature emphasizes that individual physiology, timing of use, metabolism, and hydration all influence the outcome. Because detection windows vary greatly between substances, and because certain medical conditions or medications can interfere with screening, healthcare professionals must carefully evaluate the results against the individual’s specific medical background.
Key Takeaways:
- Focus on Drug Metabolites: Urine drug tests are noninvasive, cost-effective procedures designed to detect drug metabolites rather than the original substances themselves. Since the liver produces these chemical byproducts during processing, they remain in the system much longer to provide a highly reliable indicator of recent use.
- Strict Collection and Handling: Proper sample collection requires strict chain-of-custody documentation to track handling and actively prevent legal or workplace disputes. Laboratories also perform precise validity testing on temperature, pH, and specific gravity to guarantee the specimen has not been diluted, substituted, or tampered with.
- The Initial Screening Phase: The laboratory process begins with rapid, qualitative immunoassay screenings that efficiently process large volumes of samples to flag presumptive positives. Because these biochemical tests look for specific molecular structures, they can sometimes produce false-positive or false-negative results due to cross-reactivity.
- Advanced Confirmatory Testing: Any presumptive positive results advance to highly sophisticated confirmatory testing using gold-standard methods like GC-MS or LC-MS/MS. These advanced technologies separate chemical compounds and measure exact metabolite concentrations, drastically reducing the possibility of a false positive.
- Nuanced Result Interpretation: Interpreting test outcomes requires a comprehensive analysis of the broader clinical context rather than simply reading a positive or negative label. A positive test indicates a substance exceeded the cutoff level but does not inherently prove impairment, while a negative result solely means the substance was below the reporting threshold.
FAQs:
What are the most common types of drug tests?
Urine testing is highly favored in workplaces, healthcare settings, rehabilitation programs, athletic organizations, and legal investigations because it is a relatively noninvasive and cost-effective laboratory procedure for identifying recent substance use.
What is the most accurate type of drug test?
The most accurate methods are the advanced confirmatory tests used by laboratories, specifically gas chromatography-mass spectrometry (GC-MS) and liquid chromatography-tandem mass spectrometry (LC-MS/MS).
Are all drug tests accurate?
While drug tests are highly reliable, they are not completely foolproof, as false-positive and false-negative outcomes can occasionally occur. Initial screening tests are considered presumptive because certain medical conditions, prescription medications, or over-the-counter products can interfere with the assays through cross-reactivity. To ensure greater precision, laboratories utilize a layered, two-step process.
What is the difference between a lab drug test and a regular drug test?
The first step is a rapid initial screening, typically an immunoassay test, which is qualitative and simply indicates if a substance might be present above a designated cutoff level. Because these initial screenings are considered presumptive and can sometimes produce false positives due to cross-reactivity, laboratories then employ highly sophisticated, advanced confirmatory tests, to verify the results and measure exact metabolite concentrations.
Sources.
Ayala-Lopez, N., Aref, L., Colby, J. M., & Hughey, J. J. (2021). A Computational Approach to Identify Interfering Medications on Urine Drug Screening Assays without Data from Confirmatory Testing. Journal of analytical toxicology, 45(4), 325–330. https://doi.org/10.1093/jat/bkaa140
Centers for Disease Control and Prevention. (2024, April 10). Clinical drug test dashboard. U.S. Department of Health and Human Services. https://www.cdc.gov/overdose-prevention/data-research/facts-stats/clinical-drug-test-dashboard.html
You May Also Like:
How Much Does Drug Rehab Cost Without Insurance?
How to Identify PTSD Early: What Should You Know
You survived the event, but why does the memory still dictate your daily life? For many, the aftermath of trauma doesn’t present as immediate panic, it disguises itself as sleepless nights and sudden irritability. What happens when these silent symptoms go unchecked? Discover How to Identify PTSD Early: What Should You Know and discover why joining a Mental Health Group Therapy In Brooklyn, New York, is the crucial first step toward true healing.
Access Mental Health Group Therapy In Brooklyn, New York
TL;DR:
Early PTSD often emerges shortly after a traumatic event through four main symptom categories: intrusive memories, hyperarousal, avoidance, and emotional detachment. Intrusive thoughts and vivid flashbacks severely disrupt daily functioning, while an overactivated stress system keeps the individual in an exhausting state of constant anxiety and high alert. To cope, individuals frequently avoid trauma-related triggers and emotionally detach from their loved ones, which inadvertently prevents necessary emotional processing and drives social isolation.

What are the Earliest Signs of PTSD?
The earliest signs of post-traumatic stress disorder (PTSD) often appear shortly after a traumatic event, although in some cases they may develop gradually over weeks or months. These early symptoms are typically grouped into four main categories: re-experiencing (intrusive thoughts), avoidance, heightened arousal, and changes in mood or cognition.
In the initial stages, individuals may notice subtle but persistent changes in how they think, feel, and react to their environment. These can include distressing memories of the event, increased anxiety, difficulty sleeping, or a tendency to avoid reminders of the trauma. Early symptoms are clinically important because they can indicate whether someone is at risk of developing long-term PTSD if left unaddressed.
Research also shows that early symptoms often exist on a spectrum. This means they may not meet full diagnostic criteria right away but can still significantly affect daily functioning and emotional well-being.
Intrusive Memories and Flashbacks
One of the most recognizable early signs of PTSD is the presence of intrusive memories, which are unwanted and distressing recollections of the traumatic event. These can appear suddenly and may feel vivid or overwhelming, sometimes making the person feel as if they are reliving the experience.
- Flashbacks: A more intense form of this symptom, where individuals may experience physical reactions such as sweating, rapid heartbeat, or a sense of panic, as if the danger is happening again in real time.
- Nightmares: Often replaying aspects of the trauma, neuroscientific research indicates these intrusive experiences disrupt normal sleep patterns. This reinforces emotional distress, creating a cycle where poor sleep worsens PTSD symptoms.
- Daily Impact: These symptoms are not just memories; they are emotionally charged experiences that can severely interfere with concentration, relationships, and overall daily functioning.
Heightened Anxiety and Alertness
Another early indicator of PTSD is hyperarousal, a state of constant alertness where the body remains on high warning even in safe environments. Individuals may feel tense, easily startled, or “on edge” most of the time, feeling unable to relax as if danger is always imminent.
This heightened state can manifest in several ways, including irritability, difficulty concentrating, and exaggerated reactions to sudden noises or unexpected events.
From a physiological perspective, this response is linked to the brain’s stress system remaining overactivated after trauma. This can make everyday situations feel highly threatening, even when there is no real risk. Over time, persistent hyperarousal can lead to deep fatigue, emotional exhaustion, and difficulty maintaining normal routines.
Avoidance of Trauma-Related Triggers
Avoidance is a core early symptom of PTSD and involves deliberately steering clear of anything that reminds the person of the traumatic experience.
| Avoidance Behavior | Clinical Impact |
| Physical Avoidance | Avoiding specific places, people, or activities (e.g., someone who experienced a car accident might avoid driving). |
| Psychological Avoidance | Suppressing related thoughts or entirely avoiding conversations associated with the event. |
| Long-Term Effects | While avoidance provides short-term relief, it reinforces the trauma by preventing necessary emotional processing. |
Clinically, these avoidance behaviors can gradually reshape a person’s lifestyle, limiting social interaction and daily activities. Over time, this contributes to isolation and makes recovery much more difficult.
Sleep Disturbances and Nightmares
Sleep problems are among the earliest and most persistent symptoms of PTSD. Individuals may have trouble falling asleep, staying asleep, or experience frequent awakenings during the night.
- Intensified Fear: Nightmares are particularly common and often involve direct or symbolic representations of the trauma. These recurring dreams can intensify fear and anxiety, making restful sleep nearly impossible to achieve.
- Compounding Symptoms: Sleep disturbances are significant because they not only reflect emotional distress but actively worsen other symptoms, such as irritability, concentration issues, and emotional regulation.
- Increased Vulnerability: Studies suggest that disrupted sleep may even increase a person’s vulnerability to developing more severe PTSD symptoms over time.
Emotional Numbness or Detachment
Early PTSD can also involve changes in emotional processing, particularly emotional numbness or detachment from others. Individuals may feel disconnected from their surroundings, their relationships, or even their own emotions.
This detachment can present as a reduced ability to feel happiness, love, or satisfaction, alongside persistent negative emotions such as fear, guilt, or shame. Social withdrawal is highly common, as individuals may struggle to relate to others or feel completely misunderstood. Over time, this detachment can deeply impact personal relationships and overall quality of life.
From a psychological standpoint, emotional numbness is often viewed as a coping mechanism, an attempt by the brain to protect itself from overwhelming distress. Nevertheless, when prolonged, it can hinder emotional recovery and contribute to long-term difficulties in mental health.
Key Takeaways:
- Intrusive Memories and Flashbacks: Early signs of PTSD often manifest as unwanted, distressing recollections of the traumatic event that severely disrupt daily functioning. These emotionally charged memories can escalate into intense flashbacks, triggering real-time physical reactions like sweating and rapid heartbeats.
- Heightened Anxiety and Hyperarousal: A primary physiological indicator of PTSD is a constant state of hyperarousal caused by an overactivated stress system in the brain. This heightened alertness makes completely safe, everyday situations feel highly threatening, leaving individuals perpetually on edge, irritable, and easily startled.
- The Dangers of Avoidance: Avoidance behaviors act as a core symptom where individuals deliberately steer clear of physical locations, conversations, or thoughts associated with their trauma. While this psychological suppression may provide a sense of short-term relief, it actively reinforces the trauma by preventing necessary emotional processing.
- Persistent Sleep Disturbances: Sleep problems, particularly frequent awakenings and trauma-related nightmares, are among the earliest and most persistent warning signs of the disorder. These recurring dreams compound feelings of fear and anxiety, making restful sleep nearly impossible and creating a vicious cycle of ongoing distress.
- Emotional Numbness and Detachment: Emotional numbness frequently develops as a psychological coping mechanism designed by the brain to protect itself from overwhelming distress. This detachment severely reduces an individual’s ability to feel happiness or satisfaction, leading to profound social withdrawal and persistent negative emotions like guilt or shame.
FAQs:
What is PTSD?
Post-traumatic stress disorder is a condition that typically appears shortly after a traumatic event, although it may develop gradually over weeks or months. It is characterized by early symptoms that fall into four main categories: re-experiencing the trauma through intrusive thoughts, avoidance behaviors, heightened arousal, and changes in mood or cognition.
What are the signs of PTSD?
The earliest signs usually involve subtle but persistent changes, including distressing, intrusive memories of the event, vivid flashbacks, and frequent nightmares that disrupt sleep. Other indicators are hyperarousal and deliberately avoiding places, people, or conversations that trigger memories of the trauma.
How do you confirm you have PTSD?
Confirming the risk involves recognizing persistent changes in your thoughts, feelings, and reactions, which is clinically important to identify before long-term PTSD develops. Exploring these signs in a professional setting, such as mental health group therapy, is highlighted as a crucial first step toward addressing the symptoms and finding true healing.
What does PTSD do to a person?
It significantly impacts a person’s life by turning emotionally charged memories into severe disruptions that interfere with concentration, personal relationships, and overall daily functioning. The constant state of hyperarousal causes deep fatigue, emotional exhaustion, and difficulty maintaining normal routines.
Sources.
Bonde, J. P. E., Jensen, J. H., Smid, G. E., Flachs, E. M., Elklit, A., Mors, O., & Videbech, P. (2022). Time course of symptoms in posttraumatic stress disorder with delayed expression: A systematic review. Acta psychiatrica Scandinavica, 145(2), 116–131. https://doi.org/10.1111/acps.13372
Ressler, K. J., Berretta, S., Bolshakov, V. Y., Rosso, I. M., Meloni, E. G., Rauch, S. L., & Carlezon, W. A., Jr (2022). Post-traumatic stress disorder: clinical and translational neuroscience from cells to circuits. Nature reviews. Neurology, 18(5), 273–288. https://doi.org/10.1038/s41582-022-00635-8
You May Also Like:
What Are the Six Psychological Interventions?
Recovery Home Health Care: Services, Benefits, and What to Expect
Leaving the hospital feels like the finish line, but what if the most vulnerable phase of your healing begins right in your own living room? Unseen setbacks often derail progress when the proper support is missing. Uncover the truth in Recovery Home Health Care: Services, Benefits, and What to Expect, and discover the ultimate missing link for your safe healing: expert Care Management In Brooklyn, New York.
Start Care Management In Brooklyn, New York
TL;DR:
Recovery home health care offers a multidisciplinary, patient-centered approach to healing and restoring independence safely following an illness or surgery. To prevent severe complications and hospital readmissions, a physician-directed team provides skilled nursing for vital medical monitoring and strict medication management. This clinical support is complemented by physical and occupational therapies designed to rebuild mobility, alongside specialized wound and post-surgical care to actively prevent infections.

What Services are included in Home Health Recovery Care?
Home health recovery care encompasses a broad range of medical and supportive services delivered directly in a patient’s home. Designed to promote healing, restore independence, and manage health conditions following an illness, injury, or surgery, this service is highly patient-centered. According to general government health guidelines, these services are typically provided under a physician-directed plan and involve a multidisciplinary team that may include nurses, therapists, and home health aides.
By allowing individuals to recover in a familiar environment while receiving medically necessary support, the ultimate objective goes beyond immediate recovery. It aims to maintain long-term health and prevent hospital readmissions by teaching patients and their caregivers how to safely manage ongoing care needs at home. Depending on the patient’s specific condition and goals, the plan usually includes the following core services:
Skilled Nursing and Medical Monitoring
Skilled nursing is a foundational component of home health recovery care, involving services delivered by licensed professionals such as registered nurses (RNs) or licensed practical nurses (LPNs). These services are critical when a patient requires clinical expertise that non-professional caregivers simply cannot safely provide.
In the home setting, skilled nursing tasks include:
- Monitoring vital signs and assessing health conditions.
- Managing chronic diseases and administering injections or intravenous (IV) therapies.
- Educating patients and families on proper techniques.
Nurses serve as a vital link, coordinating care with physicians and identifying early warning signs of complications to prevent hospital readmissions.
Physical and Occupational Therapy Support
Therapy services are essential for helping patients regain their function, mobility, and independence after a major health event. Depending on individual needs, home health care commonly integrates physical therapy, occupational therapy, and occasionally speech-language therapy to address physical recovery and everyday tasks.
| Therapy Type | Focus Area | Common Interventions |
| Physical Therapy (PT) | Restoring strength, balance, and movement. | Personalized exercise programs and gait training to improve mobility and reduce fall risks (often post-surgery, fractures, or neurological conditions). |
| Occupational Therapy (OT) | Relearning or adapting to daily activities. | Assistance with dressing, bathing, and using household tools, alongside recommendations for assistive devices or home modifications for safety. |
Medication Management and Administration
For patients with complex treatment regimens, medication management is a critical service. It ensures that medications are taken correctly, safely, and exactly on schedule to optimize health outcomes and reduce the risk of adverse side effects.
Structured medication oversight includes:
- Direct administration of medications by skilled nurses, including IV therapies or injections.
- Monitoring and evaluating the patient’s physical response to the treatment.
- Educating patients and their caregivers on proper dosages, timing, and potential side effects.
- Reviewing active prescriptions, coordinating with pharmacists or physicians, and making necessary adjustments.
This oversight is especially crucial for individuals recovering from surgery or managing chronic conditions, where medication errors could easily lead to severe complications or a delayed recovery.
Wound Care and Post-Surgical Care
Wound and post-surgical care are specialized interventions provided to support healing and actively prevent infections. These services are delivered by skilled nurses trained specifically in managing pressure ulcers, surgical incisions, and other complex wounds.
Professional wound care involves cleaning and dressing wounds, meticulously monitoring for signs of infection, and ensuring the healing process is progressing correctly. Under general federal health guidelines, wound care is classified as a medically necessary skilled service because it requires distinct professional expertise.
Additionally, post-surgical assistance encompasses pain management, tracking recovery milestones, and educating the patient on activity restrictions and self-care techniques. This targeted support significantly reduces post-operative complications and ensures a smoother transition from the hospital back to the home.
Daily Living Assistance at Home
Beyond direct medical interventions, home health recovery often includes crucial assistance with activities of daily living (ADLs). This is particularly important for patients struggling with limited strength or mobility. Under the supervision of skilled professionals, home health aides provide compassionate support for routine tasks.
Assistance typically covers:
- Bathing, grooming, and personal hygiene.
- Dressing and eating.
- Safe mobility around the home.
- Light household assistance, such as changing bed linens.
While these supportive tasks are not independently classified as “skilled” medical care, they are absolutely essential for maintaining a patient’s dignity, comfort, and safety. By ensuring individuals can function effectively in their daily environment, these services perfectly complement the broader clinical treatments.
Key Takeaways:
- Skilled Nursing and Medical Monitoring: Skilled nursing is a core component of home recovery, utilizing licensed professionals to manage complex needs that non-professionals cannot handle safely. These nurses monitor vital signs, administer IV therapies, and educate families on proper techniques.
- Physical and Occupational Therapy: Therapy services are critical for helping patients regain their strength, mobility, and independence following a significant health event. Physical therapy focuses on restoring movement and balance through personalized exercises and gait training to reduce the risk of falls.
- Medication Management and Administration: Structured medication oversight ensures that complex prescriptions are taken safely, correctly, and on schedule to optimize overall health outcomes. Skilled nurses directly administer necessary treatments, monitor the patient’s physical response, and educate caregivers on potential side effects.
- Specialized Wound and Post-Surgical Care: It is a medically necessary skilled service where trained nurses meticulously clean and dress surgical incisions or pressure ulcers. This specialized intervention actively prevents infections and ensures the body’s natural healing process is progressing correctly.
- Daily Living Assistance at Home: Home health recovery also includes vital support with activities of daily living for patients struggling with limited strength or mobility. Under professional supervision, home health aides provide compassionate help with essential routines like bathing, dressing, eating, and safe home mobility.
FAQs:
What are some benefits of home recovery?
Recovering at home allows individuals to heal in a familiar, comfortable environment while still receiving the medically necessary support they require. Beyond immediate healing, this patient-centered approach helps restore independence, maintain long-term health, and prevent future hospital readmissions.
What is Recovery Home Health Care?
It encompasses a broad range of medical and supportive services that are delivered directly to a patient’s home. It is designed specifically to promote healing, restore independence, and carefully manage health conditions following a significant illness, injury, or surgery.
How does Recovery Home Health Care work?
It works by utilizing a physician-directed plan that is carried out by a multidisciplinary team, which may include licensed nurses, therapists, and home health aides. Depending on the individual’s specific condition and recovery goals.
What qualifies a patient for recovery home care?
A patient typically qualifies for recovery home care when they need to manage health conditions, promote healing, or restore independence following an illness, injury, or surgery. The primary qualification is that these medically necessary services must be explicitly outlined and provided under a physician-directed plan.
Sources.
Vladeck, B. C., & Miller, N. A. (1994). The Medicare home health initiative. Health care financing review, 16(1), 7–16.
Siclovan, D. M., Bang, J. T., Yakusheva, O., Hamilton, M., Bobay, K. L., Costa, L. L., … & Weiss, M. E. (2021). Effectiveness of home health care in reducing return to hospital: evidence from a multi-hospital study in the US. International journal of nursing studies, 119, 103946. https://doi.org/10.1016/j.ijnurstu.2021.103946
You May Also Like:
How to Find a Case Manager for Mental Health Support
Depression in Prison: Causes, Symptoms, and Treatment Options
What happens when the physical bars disappear, but the invisible prison of the mind remains? For many, serving time sparks a psychological crisis that follows them long after their release. Uncover the stark reality in Depression in Prison: Causes, Symptoms, and Treatment Options, and discover why specialized Counseling For Released Inmates in Brooklyn, NY is the ultimate right path to unlocking true, lasting freedom.
Begin Counseling For Released Inmates in Brooklyn, NY
TL;DR:
Depression among incarcerated individuals is driven by the severe psychological, social, and environmental stressors inherent to prison life. The profound loss of personal autonomy and prolonged social isolation often strip individuals of their identity, breeding a state of “learned helplessness” and deep hopelessness. This emotional distress is heavily compounded by chronic exposure to violence, the grief of being separated from family support systems, and a widespread lack of accessible mental health care.

What Causes Depression in Prison Environments?
Depression in prison environments is shaped by a complex interaction of psychological, social, and environmental stressors. Research shows that incarceration itself can significantly harm mental health, sometimes leading to the development or worsening of depressive disorders.
Two main theoretical perspectives help explain this: the importation model, which suggests individuals enter prison with pre-existing vulnerabilities, and the deprivation model, which argues that the prison environment itself produces psychological distress. Modern studies emphasize that prison conditions create an environment where depression can thrive. These factors often combine, increasing risks of hopelessness, emotional withdrawal, and reduced life satisfaction. Additionally, incarceration disrupts identity, purpose, and social roles, which are essential for maintaining mental well-being.
Social Isolation and Limited Contact
Social isolation is one of the most significant contributors to depression in prison settings. Incarcerated individuals are frequently separated from meaningful relationships and may have limited opportunities for communication with family and friends.
- Disconnection: Research highlights that reduced social support and disconnection from society are strongly linked to poor mental health outcomes, including depression, loneliness, and suicidal ideation.
- Restrictive Conditions: Isolation can be intensified in restrictive conditions such as solitary confinement, where individuals may spend long periods without meaningful interaction. Studies show that lack of social stimulation and interaction is associated with increased psychological distress and depressive symptoms.
- Institutional Barriers: Even outside solitary confinement, institutional barriers, such as limited visitation, restricted phone access, or strained interpersonal dynamics, can prevent inmates from maintaining supportive relationships.
- Emotional Resilience: Over time, this lack of connection reduces emotional resilience and increases vulnerability to depression.
Loss of Personal Freedom and Control
The loss of autonomy is a defining feature of incarceration and a major psychological stressor. Prisoners have little control over their daily routines, decisions, or environment, which can lead to feelings of helplessness and reduced self-worth.
| Factor | Psychological Impact |
| Diminished Autonomy | Research identifies lack of control as an essential environmental factor associated with psychological distress in prisons. |
| Erosion of Agency | This constant restriction can erode a person’s sense of identity and ability to make basic life decisions. |
| Learned Helplessness | Being unable to make decisions may contribute to a psychological state closely linked to depression. |
| Unpredictability | The rigid structure and unpredictability of prison life can intensify stress and lead to hopelessness, a core symptom of depressive disorders. |
Exposure to Violence or Unsafe Conditions
Exposure to violence, whether direct or indirect, is another critical factor contributing to depression in prison environments. Many incarcerated individuals face threats, intimidation, or actual physical harm, creating a persistent sense of fear and insecurity.
Studies show that experiencing or witnessing violence, along with fear of victimization, significantly impacts mental health and increases the risk of depression and anxiety. Unsafe conditions, such as overcrowding, tension among inmates, and negative interactions with staff, can further amplify stress.
These environments often lead to hypervigilance, emotional exhaustion, and trauma-related symptoms, all of which are strongly associated with depressive states. Over time, chronic exposure to such stressors can make individuals feel unsafe even in non-threatening situations, reinforcing long-term psychological distress.
Lack of Mental Health Resources
Limited access to mental health care is a widespread issue in prison systems worldwide. Despite high rates of mental health disorders among incarcerated populations, only a fraction of individuals receive appropriate treatment.
- Barriers to Care: These include insufficient staffing, long wait times, stigma, and reluctance among inmates to seek help.
- Accessibility Challenges: Research indicates that even when services are available, accessibility and utilization remain significant challenges.
- Worsening Symptoms: Without proper diagnosis and treatment, depressive symptoms can worsen over time. Untreated depression may lead to self-harm, substance use, or difficulties in participating in rehabilitation programs.
- Long-Term Consequences: The lack of consistent, high-quality mental health support not only affects individuals during incarceration but also has long-term consequences for reintegration into society.
Separation from Family and Support Systems
Separation from family and loved ones is one of the most emotionally distressing aspects of incarceration. Being physically and emotionally distant from support systems can lead to intense feelings of grief, loneliness, and abandonment. Research consistently shows that disconnection from family and reduced social support are major contributors to depression among incarcerated individuals.
Family relationships often provide emotional stability, identity, and a sense of belonging. When these connections are weakened or lost, individuals may struggle to cope with stress and maintain hope for the future. Additionally, concerns about family well-being, parenting responsibilities, and relationship breakdowns can further intensify emotional distress.
The absence of supportive relationships removes a critical protective factor against depression. Making individuals more vulnerable to long-term mental health challenges, this separation deeply impacts the ability to maintain psychological well-being while incarcerated.
Key Takeaways:
- Social Isolation and Disconnection: Severe social isolation and institutional barriers, such as restricted communication and solitary confinement, strip incarcerated individuals of vital social support. This profound disconnection drastically reduces emotional resilience over time, making inmates significantly more vulnerable to deep loneliness, severe depressive symptoms, and suicidal ideation.
- Loss of Autonomy and Agency: The absolute loss of personal freedom and control over daily routines acts as a major psychological stressor in prison. Stripped of basic agency and facing rigid unpredictability, individuals often develop “learned helplessness” and a lost sense of identity.
- Exposure to Violence and Chronic Fear: Constant exposure to unsafe conditions, overcrowding, and the persistent threat of physical harm creates an environment steeped in fear and insecurity. This chronic stress forces individuals into a continuous state of hypervigilance and severe emotional exhaustion.
- Inadequate Mental Health Resources: Despite high rates of psychological distress, inmates face massive barriers to mental health resources, including severe understaffing, long wait times, and institutional stigma. Without proper diagnosis or clinical intervention, these depressive symptoms inevitably worsen rather than improve.
- Separation from Family Systems: Being physically and emotionally cut off from family removes a crucial protective factor that normally provides a sense of stability, identity, and belonging. The resulting grief, compounded by constant worry over family well-being and strained relationships, deeply intensifies emotional distress.
FAQs:
Is depression common in prison?
Yes, depression is very common in prison. Research shows that the prison environment creates psychological distress where depressive disorders can thrive due to the severe psychological, social, and environmental stressors inherent to incarceration.
How does depression affect prisoners?
Depression deeply affects prisoners by eroding their sense of identity, purpose, and self-worth. As the mental health condition worsens, it often leads to a pervasive state of hopelessness, severe emotional withdrawal, and “learned helplessness.” If left untreated, these depressive states can increase the risk of self-harm, substance use, and difficulties in participating in rehabilitation programs.
What mental health issues do prisoners manifest?
The extreme stress an isolation of the prison environment can cause inmates to manifest severe anxiety, deep loneliness, emotional exhaustion, trauma-related symptoms, and suicidal ideation.
What causes depression in prisoners?
Depression among incarcerated individuals is driven by a complex interaction of psychological, social, and environmental stressors. While some individuals enter the system with pre-existing vulnerabilities, the harsh prison environment itself actively produces psychological distress by disrupting their identity, purpose, and social roles.
Sources.
Ndindeng A. N. (2024). Mental health and well-being in prisons and places of detention. International journal of prison health, ahead-of-print(ahead-of-print), 10.1108/IJOPH-07-2024-0035. https://doi.org/10.1108/IJOPH-07-2024-0035
Favril, L., Rich, J. D., Hard, J., & Fazel, S. (2024). Mental and physical health morbidity among people in prisons: an umbrella review. The Lancet. Public health, 9(4), e250–e260. https://doi.org/10.1016/S2468-2667(24)00023-9
You May Also Like:
Prison Rehabilitation Programs: Assessing Their Impact